There’s nothing quite as unsettling as feeling like something is wrong with your body but not knowing exactly what it is. That’s where I found myself not long ago. I thought I was dealing with gallbladder issues, based on my symptoms and some lab results, but after digging deeper, the real culprit turned out to be something I hadn’t expected—fatty liver disease.
Here’s my story, from the first sign that something was off to finally getting clarity with the help of imaging and a specialist.
It Started with Elevated Bilirubin
It all began with a routine blood test. My doctor noted that my bilirubin levels were higher than normal. Bilirubin, as I later learned, is a substance produced when your body breaks down red blood cells. Normally, the liver processes bilirubin, and any excess is eliminated through bile or urine. High levels can point to various issues, including liver dysfunction or bile duct problems.
At the time, I didn’t have any glaring symptoms beyond occasional fatigue and a general sense of discomfort after eating rich meals. However, elevated bilirubin set off a cascade of questions: Was it my liver? My gallbladder? Could it be something more serious?
The “Gallbladder Issue” Theory
When I started researching my symptoms, gallbladder issues seemed like the obvious answer. I had:
- Mild abdominal discomfort: It wasn’t sharp pain but a nagging sensation in my upper right abdomen after eating fatty foods.
- Occasional nausea: Especially after heavier meals.
- Fatigue: Something that could be attributed to either gallbladder or liver problems.
Gallbladder issues, especially gallstones, can cause symptoms that overlap with liver dysfunction. Since the gallbladder and liver work closely to produce and store bile, I assumed my discomfort and elevated bilirubin were due to a gallbladder problem. It all made sense—until it didn’t.
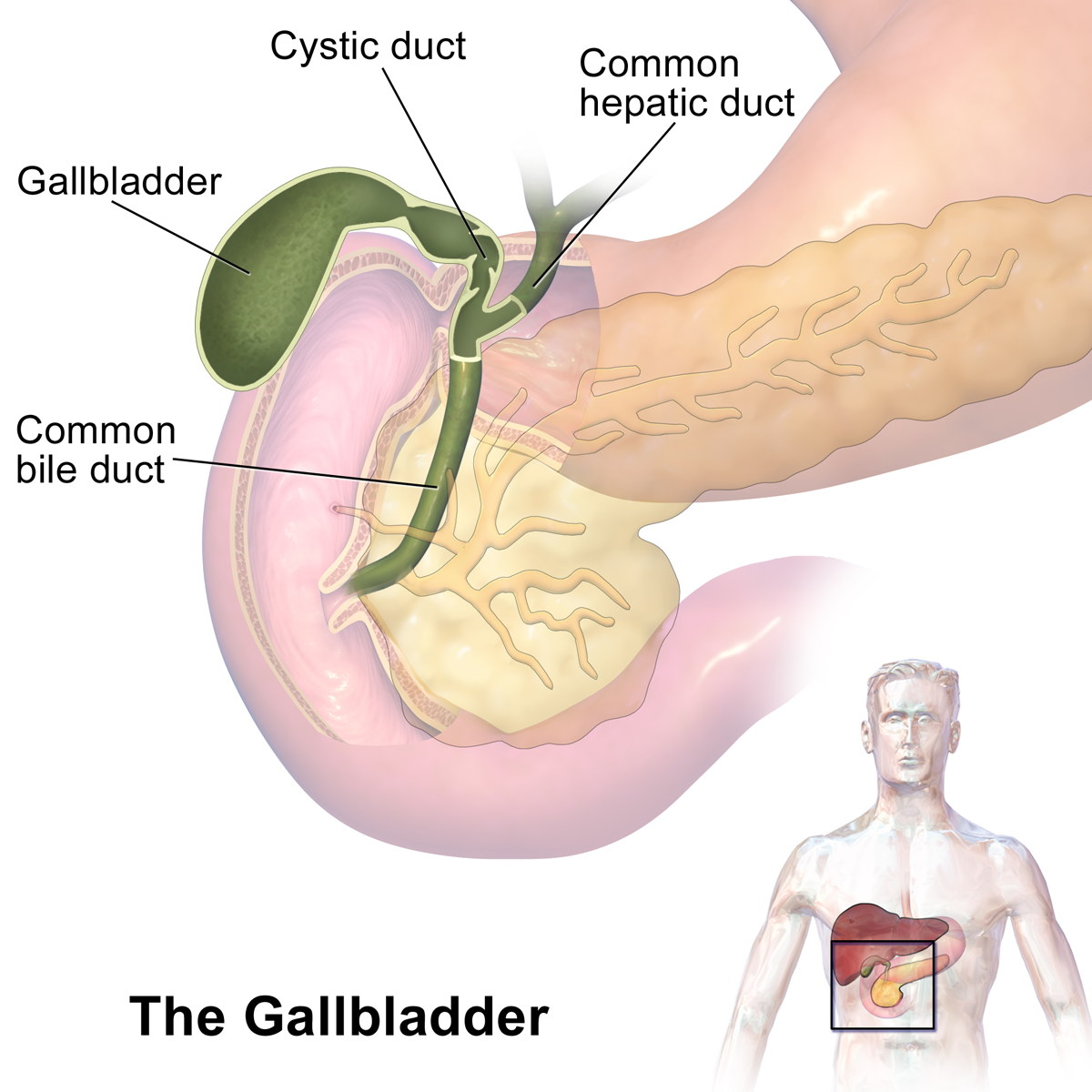
Seeing a Specialist and Getting Imaging Done
After weeks of speculation (and a lot of Googling), I decided to see a gastroenterologist. The first step was to rule out gallstones or bile duct blockages, so they ordered an ultrasound of my abdomen.
The ultrasound didn’t show any gallstones or inflammation, which left me puzzled. Was my gallbladder acting up without any visible signs? The specialist recommended further testing to dig deeper into the root cause of my symptoms. Next up was a MRI with specialized liver imaging, and that’s when the real answer started to emerge.
The Fatty Liver Diagnosis
The imaging revealed something unexpected: fat infiltration in my liver. The official diagnosis was non-alcoholic fatty liver disease (NAFLD), a condition where fat builds up in the liver cells, often without symptoms. This discovery shifted my focus entirely.
While my elevated bilirubin and mild symptoms had pointed me toward gallbladder issues, it turned out that my liver was under stress. This made sense in hindsight—NAFLD is one of the most common causes of mild liver dysfunction and elevated bilirubin levels in otherwise healthy individuals.
What I Learned About Fatty Liver Disease
I quickly learned that NAFLD is linked to lifestyle factors like diet, weight, and overall metabolic health. Some of the risk factors include:
- Being overweight or obese.
- Insulin resistance or prediabetes.
- A diet high in refined carbs and saturated fats.
- Sedentary lifestyle.
While fatty liver is often silent in its early stages, it can lead to more serious liver issues if left unchecked. For me, this was a wake-up call to prioritize my liver health.
How I Changed My Lifestyle
The diagnosis wasn’t just a label—it was a turning point. My doctor emphasized that fatty liver is reversible, especially in its early stages. With that in mind, I made several changes:
- Diet Overhaul:
- I shifted to a Mediterranean-style diet, focusing on whole foods, lean protein, healthy fats, and lots of vegetables.
- I cut back on processed foods, sugar, and saturated fats.
- Check out this SAMPLE DIET
- Incorporating Exercise:
- I started walking daily and added light weightlifting to my routine.
- Even small amounts of exercise can reduce fat in the liver and improve overall metabolic health.
- Monitoring My Progress:
- Regular follow-ups with my specialist to track liver health.
- Keeping an eye on my bilirubin levels and liver enzymes through periodic blood tests.
Why It Wasn’t My Gallbladder
Looking back, it’s easy to see how the symptoms and lab results initially pointed toward my gallbladder. The overlap between liver and gallbladder symptoms can make it tricky to distinguish between the two. However, the lack of visible issues on the ultrasound and the findings from my MRI were the key to getting the correct diagnosis.
The takeaway? Never assume. When it comes to your health, a thorough workup is essential. Gallbladder issues may seem like the obvious choice, but your liver—and your overall health—deserve a closer look.
My Message to Others
If you’re dealing with elevated bilirubin, abdominal discomfort, or other vague symptoms, don’t jump to conclusions. Work with a specialist who can run the right tests, including imaging, to get to the bottom of your symptoms. Whether it’s your gallbladder, liver, or something else entirely, the sooner you know, the sooner you can take action.
For me, what started as a suspected gallbladder issue turned into a journey of understanding my liver health. It’s been a learning experience, but one I’m grateful for. NAFLD is manageable, and with the right lifestyle changes, I’m working toward better health every day.
Your body is always speaking to you—listen to it and don’t be afraid to seek answers.cerns.

